How To Treat Phlebitis Efficiently: Proven Methods for Fast Relief
A disorder distinguished by vein inflammation, phlebitis can be unpleasant and disruptive. Usually, in the legs or arms, it arises when a vein is irritated. Usually brought on by an infection, blood clots, or extended inactivity, phlebitis is Although this can be alarming, the good news is that various effective treatments for this disorder are now at hand. Preventing problems, including blood clots or infections, depends on early treatment.
In this article, we will discuss tested strategies for treating phlebitis. We will also offer useful advice on symptom management and encouragement of healing. Understanding how to treat phlebitis will enable you to rapidly find relief from this ailment and resume your regular activities.
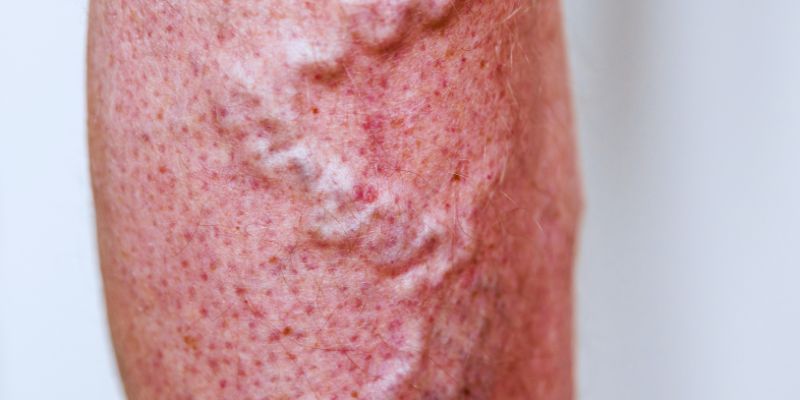
Understanding Phlebitis: Causes and Symptoms:
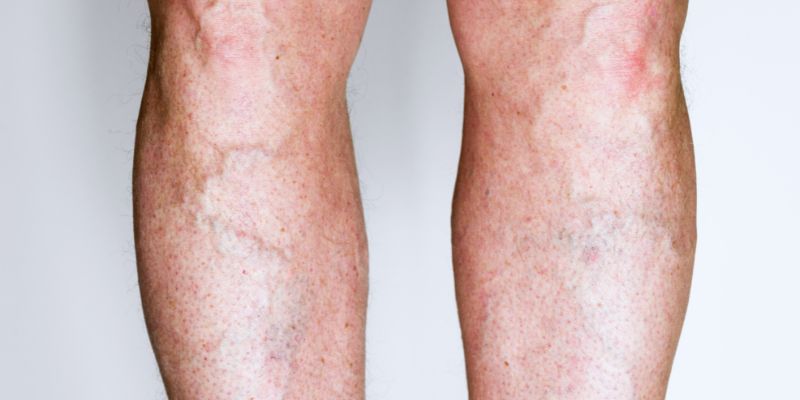
Phlebitis is when a vein becomes inflamed, usually resulting in discomfort, redness, and swelling along the vein. It can cause more severe problems in deeper or superficial veins close to the skin's surface. Phlebitis comes mostly in two forms: superficial and deep vein phlebitis. Meanwhile, deep vein phlebitis involves deeper veins and can cause major problems, including deep vein thrombosis (DVT). However, superficial phlebitis affects veins close to the surface of the skin.
Vein damage, extended immobility, or infection are common causes of phlebitis. Blood clots can also aggravate vein irritation. Redness, swelling, warmth, and soreness around the afflicted vein are among the symptoms of phlebitis. Severe occurrences might cause the skin to get hard or exhibit symptoms of infection. Early identification of these symptoms is crucial for effective treatment and prevention of further problems.
Effective Treatments for Phlebitis:
Effective treatment of phlebitis combines home remedies, lifestyle modifications, and occasionally medical intervention. Applying warm compresses to the afflicted area comes first in treatment. Heat soothes pain and helps to lower inflammation. Another important tactic is raising the afflicted limb. Maintaining an elevated leg or arm helps enhance blood flow and lower swelling, accelerating healing.
NSAIDs, including ibuprofen, help control inflammation and discomfort. They are not steroidal anti-inflammatory medications. These medicines are extensively used in the treatment of phlebitis. Should a blood clot exist, a healthcare professional could advise anticoagulant treatment to stop further clotting. Compression stockings also help treat superficial phlebitis by increasing circulation and lowering swelling.
Lifestyle Changes for Managing Phlebitis:
Adopting good lifestyle choices can greatly help manage phlebitis and stop its recurrence. Regular physical exercise improves blood circulation and lowers blood pressure risk. Easy exercises like swimming or walking may help keep veins healthy and maintain appropriate blood flow.
Those who spend much time seated or standing should make regular breaks and move about. Stretching the legs and flexing the feet can prevent blood from collecting in the veins. Reducing the pressure on veins, especially in the lower limbs, also depends on keeping a good weight. A balanced diet of antioxidants and fiber helps lower body inflammation and improve general vein condition. Moreover, being hydrated helps circulation. When paired with appropriate therapy, these lifestyle modifications can lower phlebitis risk and increase the recovery period.
Medical Treatments for Severe Phlebitis:
Sometimes, phlebitis calls for more complex medical treatment, particularly if it includes deep veins or a blood clot involvement. Often used to treat current clots or lower the risk of their formation, anticoagulants, sometimes known as blood thinners, These medicines assist in stopping the clot from growing or developing additional problems, including pulmonary embolism or deep vein thrombosis (DVT).
Doctors may advise a thrombectomy—a surgery to remove the clot—for severe phlebitis. A surgical intervention is sometimes required if the clot is big and compromises circulation. Those who experience recurrent phlebitis could want to discuss vein stripping or laser treatments. These surgeries seek to cure or eliminate the afflicted vein to stop more inflammation. Depending on the degree of the disease, always see a healthcare practitioner to ascertain the best line of action.
The Role of Compression Therapy in Phlebitis Treatment:
Compression therapy is among the most successful techniques for controlling phlebitis, particularly in cases involving superficial veins. By gently squeezing the impacted area, compression stockings or bandages improve blood flow and help lower edema. This relieves inflammation and irritation and helps the veins resume their usual operation.
Those who have varicose veins or are at risk of blood clot development can especially benefit from compression therapy. Applying constant pressure to the legs helps the blood flow more efficiently and minimizes pooling. It also lessens the likelihood of further vein irritation. Besides donning compression stockings, following correct frequency and length of use guidelines is crucial. See a healthcare professional to find the optimal kind of compression for your particular ailment.
When to See a Doctor for Phlebitis?
Although at-home therapies can help control many cases of phlebitis, there are some cases when you should see a doctor. Medical treatment is needed if the swelling and discomfort worsen, even by trying home remedies such as NSAIDs or warm compresses. Furthermore, quick medical attention is required if the impacted area exhibits symptoms of infection, including pus, redness, or warmth.
Rarely, phlebitis can create major problems, including deep vein thrombosis (DVT), which might cause extreme discomfort, swelling, or trouble breathing. See ER if you have any of these symptoms. Those with a history of blood clotting problems or other vascular diseases should also see a doctor to guarantee appropriate control. For people with recurrent phlebitis, regular follow-up visits are crucial for monitoring the disorder and modifying treatment approaches. For severe or consistent symptoms, always consult a professional.
Preventing Phlebitis: Tips for Long-Term Relief:
Preventing phlebitis requires maintaining good circulation and minimizing risk factors causing vein inflammation. Maintaining activity is among the best ways to prevent certain diseases. Regular exercise—especially activities involving the legs, such as cycling or walking—helps strengthen veins and increase blood flow. Another crucial factor is avoiding protracted periods of immobility; if you have to sit or stand long, take breaks and move about.
Compression stockings worn on extended flights or during lengthy periods of sitting can help stop blood from accumulating in the veins. Maintaining hydration and following a healthy diet with foods high in antioxidants and fiber will also help the body to be less inflammatory. Seeking medical guidance on preventative measures may help patients with a risk of phlebitis—those with a family history of vein diseases or obesity—reduce future events of the condition.
Conclusion:
Effective phlebitis treatment combines lifestyle modifications, home remedies, and, when needed, medical procedures. Early identification of symptoms and fast treatment can help to lessen pain and avoid consequences, including blood clots. Those with mild cases can effectively manage by utilizing heat, raising the impacted leg, and administering compression therapy. Medical therapies, including blood thinners or surgical operations, could be required in severe situations. Compression therapy, a good diet, and consistent exercise help to prevent phlebitis.